Many factors will determine the gain of bone whenever we are performing a Regenerative Procedure; here I will share the most important ones:
1-. Type of defect. We have a classic and more contemporary classification but the Sievert classification allows us to determine the lack of bone horizontally (I), vertically (II) or in a combination of both (III).
2-. Especially in the aesthetic zone the height of inter-proximal bone of adjacent teeth will maintain the papilla height of our final rehabilitation.
3-. The decision making process to place the implant will depend on the severity of the defect, MILD, MODERATE or SEVERE. Assuming the immediate implant placement on the first and second situations and staging on the third.
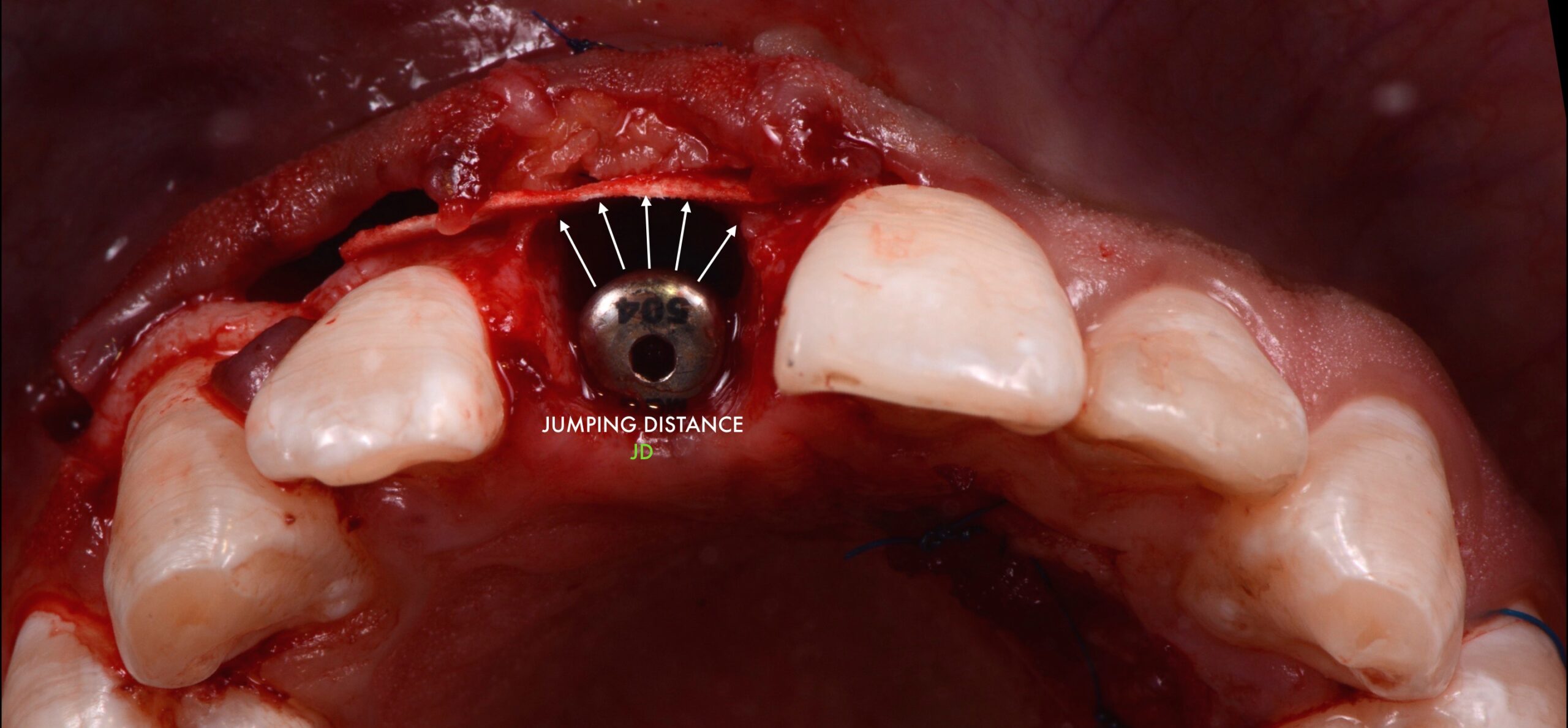
4-. The jumping distance (see the picture) will also determine the amount of regenerative potential understanding that the blood supply will reach the grafted area from the hosting bone available. Try not to overbuild out of the bone envelope, it will increase the tension of your flap and will raise the chances to experience a dehiscence.
5-. The more cancellous bone at the recipient site the more chances to predict the regeneration. Cortical bone lacks of regenerative potential, it serves just as scaffold.
6-. Corticotomies will be mandatory at the recipient site to increase the vascularity for the graft.
7-. Try to use a graft material that has a combined turn over to vital bone.
8-. Use growth factor therapy to improve the healing, manage the graft in GBR, and cover your membranes in touch with the inner side of the flap.
9-. Proper periosteum release to avoid tension of the flap.
10-. Primary closure and no pressure on the incision line to avoid dehiscence and bacterial contamination as well as isquemia of the area.
Watch the Masterclass for Predictable 3D Volume gain.