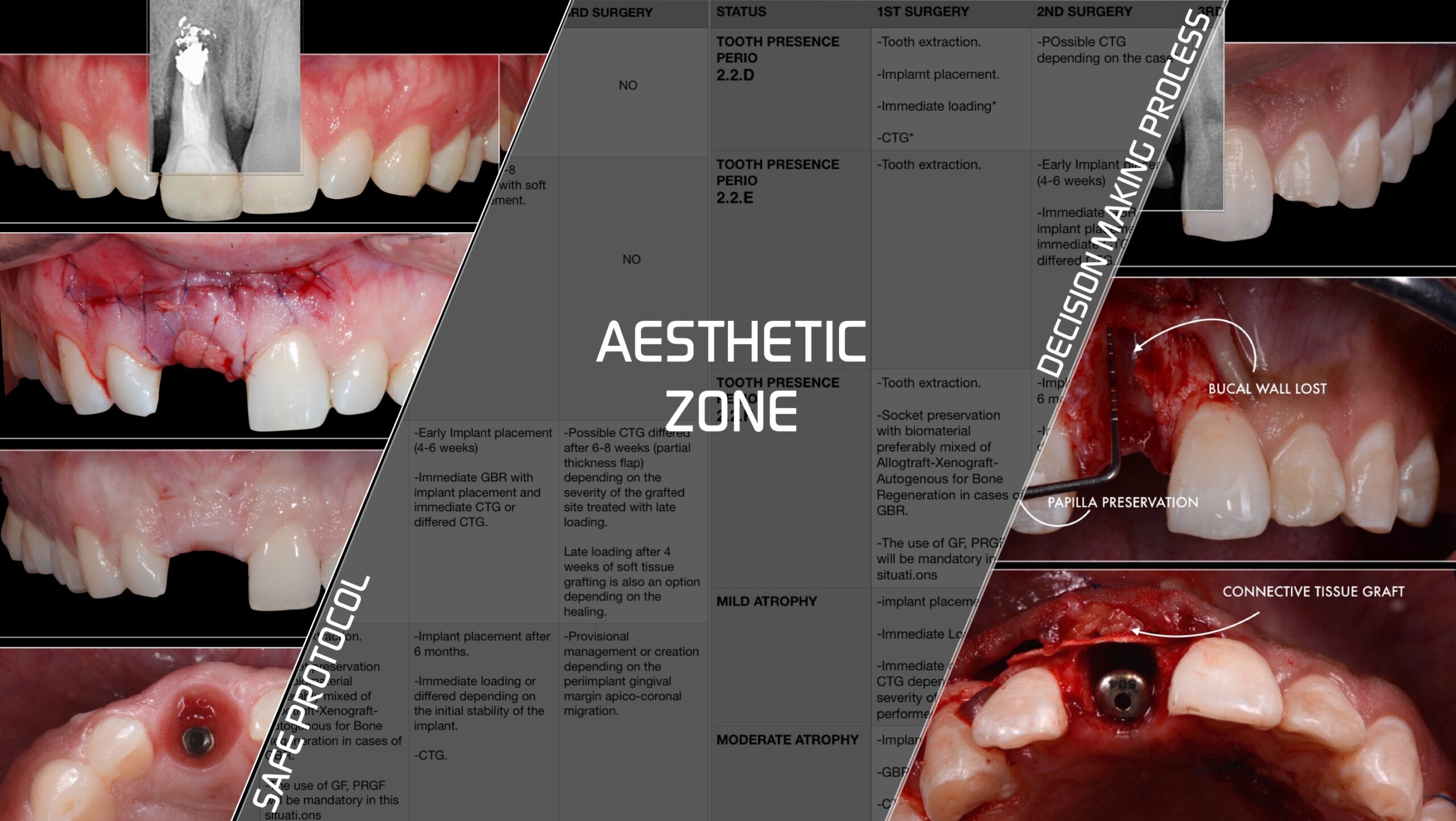
DECISION MAKING PROCESS CLASSIFICATION DSCh
Implants in the aesthetic zone. The final success will depend on this important factors:
As we all know, dental implant placement in the aesthetic zone is one of the most challenging situations we may face today, especially those with high lip line or gummy smiles, thin biotypes, and at young ages.
The warranty of gingival and bone architecture stability at long term will depend on many factors, which we will explain today according to scientific literature & clinical experience.
All this indications are described with a main goal which is not to expose yourself to unnecessary risks by trying to follow a style, trend or tendency. And only to respect the biology, which even respected in many cases the results may vary from patient to patient.
1-. Patient clinical status and reason for extraction or loss of tooth.
The patient clinical status and the case selection will be an indicator for our diagnosis & treatment planning.
From among multiple situations that we may face at the time of receiving a patient with an immediate emergency (accidental trauma / periodontal deterioration) or by aesthetic demand (old tooth loss) we can classify the situations into:
A-. Accidental trauma with bad prognosis of the tooth: Those cases that do not warranty the stability at long term of the restoration provided, e.g. Vertical Fracture, Subcrestal Horizontal fracture violating the biologic width.
B-. Severe Periodontal Disease with acute or chronic affection that generates or not a severe bone loss from the neighboring teeth.
C-. Old tooth loss with mild, moderate or severe bone loss according to:
C.1: Long time since the tooth was lost.
C.2: Buccal Bone loss by wrong surgical management during the extraction.
C.3: Periodontal Disease developed until its tooth removal which reveals an affected severe residual alveolar bone.
2-. Clinical status of the area to treat:
2.1: Lack of mobility nor periodontally affected.
2.1.A -. Presence of the tooth with buccal plate preserved and inter proximal bone intact as well as soft tussle levels. . (Socket Type I).
2.1.B -. Presence of the tooth with loss of buccal plate and inter proximal bone intact as well as soft tussle levels. (Socket Type II).
2.1.C -. Presence of the tooth with loss of buccal plate and soft tissue levels apically migrated. Inter proximal bone intact. (Socket Type III).
2.1.C.1 -. Presence of the tooth with loss of buccal plate and soft tissue levels apically migrated. Inter proximal bone affected. (Socket Type IV).
2.2: Mobility presented and periodontal disease active:
2.2.D -. Presence of the tooth with periodontal disease, inter proximal bone intact as well as soft tussle levels.
2.2.E -. Presence of the tooth with periodontal disease, inter proximal bone intact but soft tussle levels apically migrated.
2.2.F -. Presence of the tooth with periodontal disease, inter proximal bone affected and soft tussle levels apically migrated.
2.3: Absence of the tooth and different atrophic degrees:
2.3.A -. Mild atrophy: Loss of 1-2 mm in B-L direction (Sievert I)
2.3.B -. Moderate atrophy: Loss of 3-4 mm in B-L direction (Sievert II)
2.3.C -. Severe atrophy: Loss of more than 4 mm in B-L direction or apicocornal (Sievert III)
3-. Based on this parameters we will create our treatment planning which will guide our Surgical Predictable Plan following the most predictable steps to avoid complications taking into account:
1-. Regenerative Potential.
2-. Minimal trauma and reduced number of surgeries when possible.
3-. Medical Patient conditions and case selection.
4-. Predict the biological evolution based on all this factors.
We must know the limitations of every case and follow the biology, assuming the potential risk when we are stepping away from the safe protocols.
The classification & treatment planning for each case is revealed in this Table below for the right decision making process.
Learn when, why and how to perform such a surgical procedure in the most predictable way to become more predictable and avoid complications.